With an estimated 158,850 new cases of colorectal cancer projected for 2026 in the United States alone, the transition from a diagnosis to a treatment plan can feel like an overwhelming journey into the unknown. It’s completely natural to feel anxious about how gastrointestinal cancer surgery might affect your digestive function or your ability to return to the activities you love. You deserve a treatment plan that pairs cutting-edge medical technology with a compassionate, human-centered approach to healing.
This guide will help you understand the latest surgical innovations, including the Medtronic Hugo™ robotic-assisted system that debuted in U.S. clinical use in February 2026. We’ll demystify the differences between robotic and laparoscopic options while explaining how March 2026 NCCN guideline updates for biomarker testing ensure your care is personalized to your specific needs. You’ll gain a clear roadmap for your recovery journey, focusing on how we combine robotic precision with a multidisciplinary strategy to restore your health and quality of life.
Key Takeaways
- Understand why a collaborative, multidisciplinary approach is the essential foundation for successful gastrointestinal cancer surgery and long-term clinical outcomes.
- Learn about specialized organ-sparing techniques and procedures like the Whipple procedure or colorectal resection that aim to preserve your digestive function.
- Discover how the marriage of robotic precision and the surgeon’s human touch can minimize your recovery time while maximizing surgical accuracy.
- Identify the critical steps in “prehab” and post-operative care that transform a clinical procedure into a holistic pathway for restoring your quality of life.
- Gain clarity on the specific criteria for selecting a surgical oncologist, ensuring your care is managed by experienced hands in a high-volume clinical setting.
Understanding Gastrointestinal Cancer Surgery: A Multidisciplinary Foundation
Gastrointestinal cancer surgery is a highly specialized branch of surgical oncology that focuses on treating malignancies within the digestive tract. While a diagnosis can feel like a heavy burden, it’s essential to understand that surgery remains the most effective curative treatment for the majority of these conditions. Modern medical advancements have shifted the focus from merely removing a tumor to a more sophisticated goal: achieving a complete cure while preserving as much healthy tissue and digestive function as possible. This approach ensures that the procedure isn’t just a clinical milestone but a definitive step toward restoring your quality of life.
Precision is the hallmark of modern surgical practice. We no longer view surgery as a standalone event but as a carefully timed intervention within a broader strategy. By utilizing advanced imaging and molecular testing, we can map out a gastrointestinal cancer surgery plan that respects the delicate balance of your internal anatomy. This methodical focus on detail reduces the physical impact on your body, allowing for a faster return to your daily routines and personal wellness. Our goal is to replace uncertainty with a structured, actionable solution that prioritizes your long-term health.
What is GI Surgical Oncology?
General surgery covers a broad range of abdominal issues, but GI surgical oncology requires a deeper level of specialization. With over 25 years of experience in managing complex abdominal cases, a specialist understands the intricate anatomy and the aggressive nature of digestive cancers. This field encompasses a wide scope, including the esophagus, stomach, liver, pancreas, and colon. For instance, a bowel resection might be necessary for colorectal issues, requiring precise techniques to ensure the remaining sections function correctly. By focusing on these specific organs, a surgical oncologist can apply the latest innovations to provide outcomes that go beyond traditional methods.
The Role of the Multidisciplinary Team
We don’t approach your care in isolation. The most successful outcomes arise from a multidisciplinary team (MDT) where surgeons collaborate with medical oncologists, radiologists, and pathologists. This collective expertise allows us to create a personalized treatment plan that might involve perioperative systemic therapy, a trend that is becoming the preferred standard in 2026 for gastric and esophageal cancers. By reviewing imaging and pathology reports together, we ensure every angle of your health is considered before the first incision is made. The multidisciplinary team approach is the gold standard for modern cancer care, providing a safety net of experts who are all focused on your recovery.
Specialized Surgical Interventions for GI Malignancies
Every organ within the digestive tract presents a unique anatomical challenge. When performing gastrointestinal cancer surgery, we tailor our approach to the specific biology of the tumor and the surrounding tissue. This organ-sparing philosophy is central to our practice. It ensures that the primary goal of cancer removal doesn’t compromise your long-term digestive health. By focusing on the preservation of function, we bridge the gap between clinical success and your personal well-being.
Upper GI Procedures: Esophagus and Stomach
The esophagus and stomach are vital for your nutritional wellness. Stomach Cancer Treatment often involves either a partial or total gastrectomy, depending on the tumor’s location. Our focus remains on reconstructive precision, ensuring that the connection between the esophagus and the remaining digestive tract is secure. This methodical approach allows you to maintain adequate nutritional intake as you recover, which is essential for your body’s healing process. Whether performing an esophagectomy or a gastric resection, the goal is always to restore a functional pathway for food.
Hepatopancreatobiliary (HPB) Surgery
Surgery involving the liver and pancreas requires a high degree of technical mastery. A Liver Resection can successfully remove primary or metastatic tumors, taking advantage of the liver’s unique ability to regenerate. For pancreatic head tumors, we perform the Pancreaticoduodenectomy (Whipple Procedure). This operation involves a sophisticated reconstruction of the digestive tract. Because these organs sit near major blood vessels, the surgeon’s steady hand and methodical pace are your greatest allies in achieving a safe, curative outcome.
Colorectal Cancer Resection
With an estimated 158,850 new cases of colorectal cancer projected for 2026, the need for precise interventions is greater than ever. In a Colorectal Cancer Resection, we focus on removing the malignancy while preserving the natural function of the bowel. We utilize meticulous lymph node dissection and advanced stapling technologies to reduce the risk of recurrence and ensure a secure connection. This careful approach helps maintain bowel continuity, which is a critical factor in your future quality of life. If you’re seeking a personalized evaluation of your options, consulting with a specialist can provide the roadmap you need for your gastrointestinal cancer surgery journey.
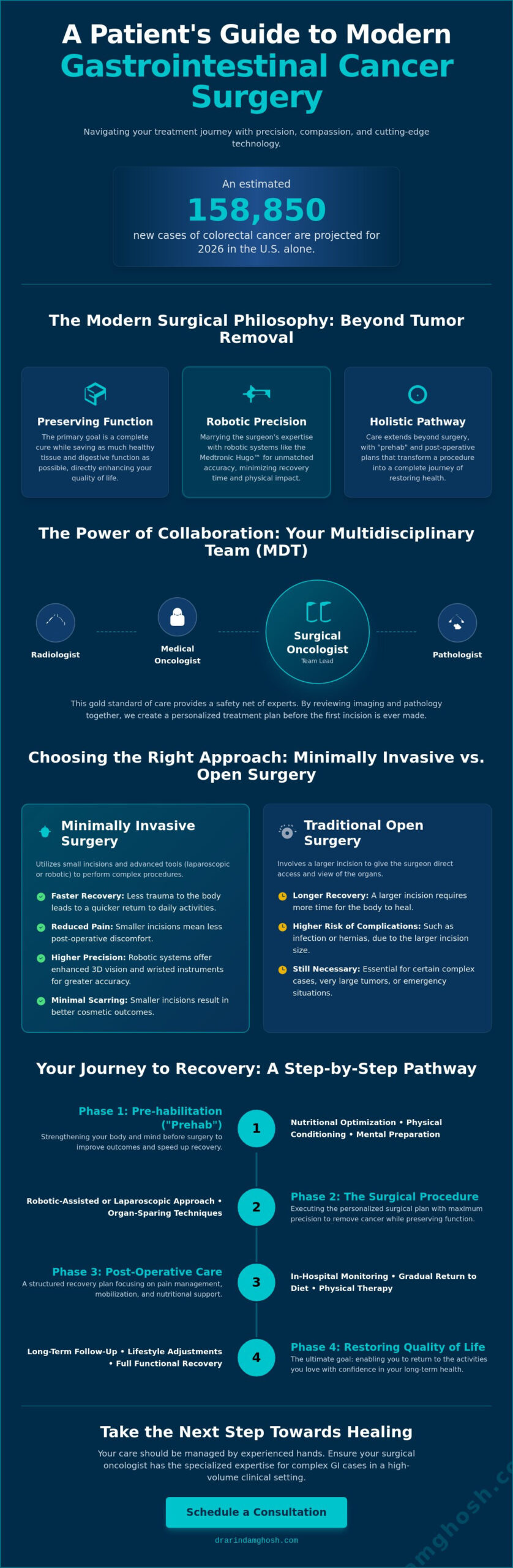
Minimally Invasive vs. Traditional Open Surgery: Choosing the Right Approach
Choosing the right surgical approach is a pivotal moment in your treatment journey. While the evolution of technology offers exciting new paths, the primary goal of gastrointestinal cancer surgery remains unchanged: achieving complete oncological clearance. Whether we use a traditional open incision or a modern robotic platform, the priority is always the thorough removal of the malignancy while preserving your long-term wellness. The decision isn’t about which tool is the “newest,” but which method offers the safest and most effective outcome for your unique anatomy, tumor location, and overall health.
We view every procedure as a marriage of the surgeon’s human touch and advanced robotic precision. This balanced perspective ensures that we don’t just treat a diagnosis; we treat a person. By tailoring the technique to the individual, we can minimize physical trauma without compromising the clinical rigor required for cancer care. The ultimate success of the operation is measured by your ability to return to a meaningful life, free from the burden of disease.
The Precision of Robotic-Assisted Surgery
Robotic-assisted surgery represents a significant leap in our ability to perform delicate dissections in complex areas. By utilizing 3D high-definition visualization, I can see tissues with a level of clarity that far exceeds the naked eye. The wristed instruments mimic the human hand’s range of motion but with a degree of stability that eliminates even the smallest natural tremor. This is especially vital in narrow, restricted spaces like the pelvis. It’s essential to understand that the robot doesn’t perform the surgery; it’s a sophisticated instrument entirely led by the surgeon’s expert hands. Key benefits of this approach include:
- Significantly smaller scars and improved cosmetic outcomes.
- Reduced blood loss during the procedure.
- Lower risk of post-operative infection.
- A faster return to your daily activities and family life.
Laparoscopic Techniques and Open Surgery
Laparoscopic surgery, often referred to as “keyhole” surgery, has been the dependable standard for many GI cases for decades. It offers a minimally invasive alternative that balances recovery speed with high clinical efficacy. The same minimally invasive principles that make laparoscopic cholecystectomy so effective for gallbladder removal are applied throughout our GI surgical practice to reduce recovery time and improve patient outcomes. However, there are specific instances where traditional open surgery remains the safest choice. For very large tumors or complex cases where a malignancy has affected multiple surrounding organs, the direct access of an open approach is necessary. We don’t let the desire for a smaller incision outweigh the necessity of a complete cure. If a tumor’s size or location makes a minimally invasive approach less certain, we transition to the traditional method to ensure the most comprehensive removal. The surgeon’s clinical judgment and experience are the most critical factors in any gastrointestinal cancer surgery, regardless of the tools used.
The Patient Journey: Preparation, Recovery, and Restoring Quality of Life
The decision to undergo gastrointestinal cancer surgery is much more than a clinical event; it’s the start of a transformative journey toward wellness. We view this procedure as a bridge that leads you away from the uncertainty of a diagnosis and toward a meaningful, healthy existence. By shifting the focus from the disease to the person, we ensure that every step of the process is designed to protect your dignity and restore your vitality. Our approach combines technical mastery with a commitment to your long-term quality of life.
Success in surgical oncology isn’t just measured by the time spent in the operating room. It’s defined by how well you’re prepared beforehand and how supported you feel during your recovery. By integrating modern clinical protocols with personalized care, we provide a structured roadmap that empowers you to take an active role in your own healing process.
Pre-operative Optimization and Planning
Preparation begins long before the day of the procedure through a process called prehabilitation. Prehabilitation is a key factor in surgical success, as it focuses on strengthening your body to better handle the physical demands of surgery. This phase includes tailored nutritional counseling to optimize your immune system and physical activity regimens to improve cardiovascular health. During our detailed pre-surgical consultations, we review the March 2026 NCCN guideline updates regarding biomarker testing, ensuring your surgical plan is perfectly aligned with your tumor’s specific molecular profile. This level of planning reduces anxiety by replacing the unknown with a clear, actionable strategy.
Post-operative Care and Nutrition
In our practice, we utilize Enhanced Recovery After Surgery (ERAS) protocols, which are the standard in advanced national centers as of 2026. These protocols prioritize early mobilization and specialized pain management techniques that reduce the need for heavy sedation. Managing your diet is a collaborative effort; our multidisciplinary team provides a step-by-step nutrition plan to help your digestive system adapt after stomach or bowel procedures. Most patients can expect a structured timeline for returning to social activities, typically within 4 to 8 weeks, depending on the complexity of the intervention. To begin building your personalized recovery plan, you can schedule a comprehensive consultation to discuss your specific roadmap.
Long-term Quality of Life
Survivorship is a lifelong commitment to your health. Beyond the initial recovery, we maintain a steady rhythm of surveillance and follow-up care to ensure your long-term wellness. This holistic support addresses the emotional journey of life after cancer, providing a sense of safety and continuity. We don’t just aim for the successful completion of a clinical task; we aim for your return to a life filled with purpose and health. Your quality of life is the thematic anchor of everything we do, serving as the ultimate goal of every surgical intervention.
Selecting an Expert GI Surgical Oncologist for Complex Care
Selecting the right specialist for your gastrointestinal cancer surgery is the most critical decision you’ll make following a diagnosis. This choice isn’t just about finding a technician; it’s about identifying a mentor and protector who will guide you through the complexities of recovery. Research consistently shows that patients who receive care at high-volume centers, where surgeons perform these procedures frequently, experience fewer complications and better long-term outcomes. By placing your trust in experienced hands, you’re ensuring that every nuance of your case is handled with the deliberate care it deserves.
A surgeon’s expertise acts as a safety net, bridging the gap between a daunting diagnosis and a successful return to your daily life. It’s essential to find a professional who views surgery not as an isolated clinical task, but as a vital part of a comprehensive, multidisciplinary strategy for your wellness. This collaborative approach ensures that your treatment is scientifically grounded while remaining deeply personal to your specific needs. If you are based in the Emirates and want to understand what a gastrointestinal surgeon does in the UAE and how to access expert care, a dedicated patient guide can help clarify the specialized roles and advanced procedures available within the region’s world-class healthcare system.
Essential Credentials and Experience
Experience is the foundation of surgical excellence. You should seek a surgeon with 20+ years of specialized experience in gastrointestinal oncology. This level of seasoning allows for a methodical and precise approach to even the most challenging malignancies. It’s essential that your surgeon is proficient in both robotic-assisted and laparoscopic techniques, as this versatility allows for a truly personalized treatment plan. Practicing in premier, internationally accredited hospitals further guarantees that the surgical team has access to the most advanced diagnostic and perioperative resources available in 2026. For a deeper look at these requirements, you can read our guide on Choosing a GI Oncologist: A Guide to Advanced Cancer Care.
The Importance of Patient-Centric Care
A surgeon’s role extends far beyond the operating theater. You deserve a physician who balances clinical authority with a compassionate, human-centric perspective. Identifying a healer who prioritizes wellness and personalized care is vital for your emotional peace of mind. During your consultation, the rhythm of the conversation should feel unhurried and measured. This steady pace reflects a physician who values your questions and respects your individual journey. It’s this blend of high-tech precision and high-touch compassion that leads to a successful restoration of your health. To begin this collaborative process, you can schedule a professional consultation with Dr. Arindam Ghosh to discuss your surgical options and create a roadmap for your future.
Restoring Your Health Through Specialized Care
Your path to recovery is defined by the choices you make today. Modern gastrointestinal cancer surgery has evolved into a sophisticated discipline where robotic precision meets a compassionate, human touch. By prioritizing a multidisciplinary approach and utilizing advanced prehabilitation strategies, we ensure that your body is prepared for the procedure and supported throughout the entire healing process. These clinical advancements are designed to replace uncertainty with a structured, actionable roadmap for your wellness.
Success isn’t just about the successful removal of a tumor; it’s about returning to the activities and people you love. With over 25 years of specialized surgical experience and deep expertise in both robotic and laparoscopic techniques, I am dedicated to protecting your future health. Every decision we make is centered on the goal of restoring your long-term quality of life through meticulous, patient-centered care.
You don’t have to navigate this complex journey alone. Consult with Dr. Arindam Ghosh for Expert GI Cancer Care and take the first step toward a personalized treatment plan built on clinical excellence and empathy. Your health is a collaborative journey, and we’re here to guide you toward a full and meaningful recovery.
Frequently Asked Questions
Is gastrointestinal cancer surgery considered major surgery?
Yes, most gastrointestinal cancer surgery is classified as major abdominal surgery because it involves the removal or reconstruction of vital organs like the stomach, liver, or pancreas. These procedures require general anesthesia and a specialized surgical oncology team to ensure safety. This clinical gravity is why we utilize a multidisciplinary approach to monitor every aspect of your physiological response during and after the procedure.
What is the typical recovery time after laparoscopic GI surgery?
Typical recovery time for laparoscopic procedures allows patients to return to light daily activities within 2 to 4 weeks. Full physical restoration usually takes 6 to 8 weeks, which is significantly faster than the 12 weeks often required for open surgery. We follow Enhanced Recovery After Surgery (ERAS) protocols to help you regain your strength and digestive function as quickly as possible.
Can robotic surgery be used for all types of GI cancers?
Robotic-assisted platforms can be used for many GI malignancies, including colorectal and gastric cancers, but the decision depends on the tumor’s size and location. As of February 2026, systems like the Medtronic Hugo™ have expanded these options for patients. However, if a tumor is exceptionally large or involves multiple major blood vessels, a traditional open approach may be the safer choice for complete oncological clearance.
Will I need chemotherapy in addition to GI cancer surgery?
Many patients receive chemotherapy or immunotherapy as part of a comprehensive plan. Following the March 2026 NCCN guideline updates, perioperative systemic therapy is now preferred for localized gastric and esophageal adenocarcinomas. This means treatment often occurs both before and after your gastrointestinal cancer surgery to improve long-term outcomes and reduce the risk of the cancer returning to the digestive tract.
What are the risks associated with complex GI procedures like the Whipple?
The Whipple procedure is a complex intervention with risks that include pancreatic juice leakage, infection, or delayed stomach emptying. In high-volume centers, the mortality rate for this procedure is typically below 5% due to specialized expertise. We manage these risks through meticulous surgical technique and a dedicated post-operative care team focused on maintaining your digestive stability and long-term quality of life.
How does surgery for stomach cancer affect my ability to eat?
Surgery for stomach cancer, such as a partial or total gastrectomy, requires you to eat smaller, more frequent meals throughout the day. Your body must adapt to a reduced storage capacity, which involves working with a dietitian to ensure proper nutrient absorption. Most patients successfully transition to a comfortable “new normal” diet within 3 to 6 months while maintaining their overall wellness.
What is the success rate for gastrointestinal cancer resection?
Success rates for resection are highest when the disease is caught in early stages. For localized colorectal cancer, the 5-year survival rate is approximately 91% according to recent oncology data. Achieving clear surgical margins is the most critical factor in a curative outcome. Our goal is always the complete removal of the malignancy to provide the best possible pathway for long-term health.
How do I prepare my body for a major abdominal operation?
Preparing for surgery involves a process called prehabilitation, which focuses on strengthening your body before the procedure. This includes increasing your protein intake for tissue repair and engaging in moderate exercise for at least 150 minutes per week. These steps strengthen your heart and lungs, which research shows can reduce post-operative complications by up to 30% in complex surgical cases.


One comment
Pingback: Choosing a GI Oncologist in Dubai: A Guide to Advanced Cancer Care